Gastroscopy
(Upper Endoscopy)
WHAT IS A GASTROSCOPY?
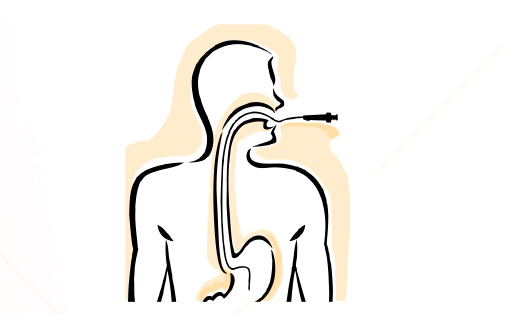
This procedure involves an endoscope – a long, thin flexible tube with a ‘video camera’ at the tip – being passed through the mouth into the oesophagus, stomach and first part of the small bowel. It allows the doctor to inspect these areas as well as perform specialised procedures such as biopsies. A gastroscopy is performed as day surgery in hospital.
This test is performed to investigate symptoms such as bleeding, pain, nausea and difficulty swallowing.
WHY IS A GASTROSCOPY DONE?
A gastroscopy is usually performed to evaluate symptoms of indigestion, upper abdominal pain, nausea, vomiting or difficulty swallowing. It is also the best test for finding the cause of bleeding from the upper gastrointestinal (GI) tract.
A gastroscopy is more accurate than x-rays for detecting inflammation, ulcers or tumours in the upper GI tract. Biopsies (samples of tissue) can be taken to determine sites of infection, to test the functioning of the small bowel and to diagnose abnormal tissue, including conditions such as coeliac disease and cancerous lesions.
A gastroscopy is also used to treat conditions of the upper GI tract. Your doctor can pass small instruments through the endoscope to directly treat many abnormalities with little or no discomfort. For example, your doctor might stretch a narrowed area, remove polyps (usually benign growths) or treat bleeding.
HOW DO I PREPARE FOR A GASTROSCOPY?
An empty stomach is essential for a safe and accurate examination, so you should have nothing to eat or drink, including water, for approximately six hours before the examination. Your doctor will provide more specific details about this, depending on the time of day that your test is scheduled.
Tell your doctor in advance about any medications you take. You might need to adjust your usual dose for the examination – this is particularly important if you have diabetes. Discuss any allergies to medications, and medical conditions such as heart or lung disease.
HOW IS A GASTROSCOPY PERFORMED?
Before the procedure a light anaesthetic (sedative) is usually given – you will not receive a full general anaesthetic. You may be slightly aware of what is going on in the room, but generally you won’t remember anything. The back of your throat may be sprayed with local anaesthetic to make it numb, and a small mouthguard may be put between your teeth to stop you from biting the endoscope. If you have false teeth (dentures) they will be removed before the procedure. The doctor and medical staff monitor your vital signs during the procedure and will attempt to make you as comfortable as possible.
The procedure takes about 15 to 30 minutes.
Once sedated and lying in a comfortable position on your left side, the endoscope is passed through the mouth and then in turn through the oesophagus, stomach and duodenum. The tube is just less than one centimetre in diameter and does not enter your windpipe, so it won’t interfere with breathing. A small camera in the end of the scope transmits a video image to a monitor, allowing the doctor to carefully examine the lining of your upper GI tract.
WHAT HAPPENS AFTER A GASTROSCOPY?
You will be monitored in the recovery area until most of the effects of the sedation medication have worn off. Your throat might be a little sore, and you might feel bloated because of the air introduced into your stomach during the test. You will be able to eat after you leave unless your doctor instructs you otherwise.
In most circumstances your doctor will briefly inform you of your test results on the day of the procedure. A follow-up appointment may be made to discuss the test results more fully. The results of any biopsies or samples taken will take several days.
Because of the sedation it is very important that you do not drive a car, travel on public transport alone, operate machinery, sign legal documents or drink alcohol on the same day after the test. It is strongly advised that a friend or relative take you home and stay with you.
Full recovery is expected by the next day. Discharge instructions should be carefully read and followed.
ARE THERE ANY RISKS OR SIDE-EFFECTS?
Although complications can occur, they are rare when the procedure is performed by doctors who are specially trained in how to perform a gastroscopy. In Australia, very few people experience serious side-effects from a gastroscopy.
The chance of complications depends on the exact type of procedure that is being performed and other factors including your general health.
You may have a slightly sore throat after the procedure and there is a slightly increased risk of chest infection. Air may also be trapped in your stomach causing you to feel bloated. If a biopsy has been taken or treatment performed, there may be minor bleeding. Very rarely, the stomach lining may be torn, and if this occurs you will be admitted to hospital for an operation to repair it.
Reactions to the sedative are also possible, but again rare.
In a few cases, if the gastroscopy is not successfully completed it may need to be repeated.
If you have any of the following symptoms in the hours or days after the gastroscopy you should contact the hospital or your doctor’s rooms immediately:
- Fever
- Trouble swallowing
- Increasing throat, chest or abdominal pain
- Other symptoms that cause you concern
WHO CAN I CONTACT IF I HAVE ANY QUESTIONS?
If you have any questions or need advice, please contact Gippsland Gastroenterology.
TAKE HOME POINTS
- A gastroscopy is a procedure used to see inside the oesophagus, stomach and first part of the small bowel
- An empty stomach is essential for a safe and accurate examination
- During a gastroscopy a light anaesthetic is often used to keep the patient comfortable
- The doctor will usually remove polyps and biopsy abnormal-looking tissue during the gastroscopy
- Driving is not permitted for 24 hours after a gastroscopy to allow the sedative time to wear off
Digestive Health Foundation Disclaimer
This information leaflet has been designed by the Digestive Health Foundation (DHF) as an aid to people who will undergo gastroscopy or for those who wish to know more about it. This is not meant to replace personal advice from your medical practitioner.
The DHF is an educational body committed to promoting better health for all Australians by promoting education and community health programs related to the digestive system.
The DHF is the educational arm of the Gastroenterological Society of Australia (GESA), the professional body representing the specialty of gastrointestinal and liver disease. Members of the Society are drawn from physicians, surgeons, scientists and other medical specialties with an interest in gastrointestinal (GI) disorders. GI disorders are the most common health-related problems affecting the community.
Research and education into gastrointestinal disease are essential to contain the effects of these disorders on all Australians.
Further information on a wide variety of gastrointestinal conditions is available on our website.